Heartburn is a common problem, but one which often has a complex cause. Today we see adverts for heartburn medication almost all the time – they suggest that just taking their simple one stop solution will resolve the problem for you, but unfortunately this isn’t always true. Even where heartburn medications are effective, there are often side effects which can sometimes be worse than the heartburn!
Today, lets look at how we can treat heartburn naturally, by addressing the underlying cause.
What Is Heartburn anyway?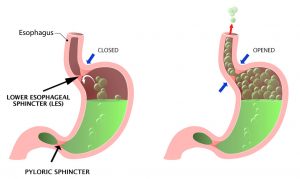
Heartburn is a common condition – very common. ln fact, a study in the journal Lancet found that one in four people in Western countries suffer from heartburn at least once per month Frequent heart burn is usually a symptom of GERO (gastroesophageal reflux), although other conditions, such as hiatal hernia, are related to heartburn.[1]
Normally, when we eat or drink, the oesophageal sphincter – a circular band of muscle around the bottom of the oesophagus -relaxes to allow food and liquid to travel down into the stomach, then closes again. But if the oesophageal sphincter isn’t working properly, stomach acid can flow back up into the oesophagus, causing what we know as heartburn.
Heartburn typically manifests as a burning sensation in the upper abdomen and chest or even the back of the throat, jaw, arms and back. It usually feels worse when lying down or bending forward.
So what’s wrong with heartburn medication?
Like all drugs, heartburn medication comes with a list of potential side effects – for the occasional treatment of infrequent heartburn the risk is probably low, but like any condition, long term treatment with medication tends to lead to side effects eventually. Popular medications include antacids, H-2 receptor blockers and proton pump inhibitors.
It’s also important to realise that some other medications can cause heartburn – if you’re taking one of the following, start there!
- Antihistamines
- Asthma medications
- NSAIDS
- Aspirin
- Antibiotics
- Heart medications
- Anti-anxiety medications
- Osteoporosis medications
- Steroids
- Chemotherapy drugs
- Anticholinergics
- Narcotic Pain releivers
Antacids
Antacids work by neutralising the stomach acid. The active ingredients in antacids are typically one or more of the following: magnesium, aluminium hydroxide, sodium bicarbonate or calcium carbonate.
Firstly, antacids may instigate problems for people with certain conditions or taking certain medications. For instance, individuals who have high blood pressure or are on a sodium-restricted diet should not take antacids containing sodium bicarbonate due to the high sodium content.
People with kidney stones should not take calcium carbonate antacids because they may exacerbate kidney problems. Also, the combination of antacids and certain drugs can lead to serious health disorders. Drugs that should not be taken in conjunction with antacids include tetracycline, indornethacin , buffered and non-buffered aspirin, iron supplements, digoxin, quinidine, Valium and corticosteroids.
In addition, overuse of some antacids can cause gastrointestinal side effects, such as diarrhoea or constipation, and calcium carbonate based produces might actually worsen heartburn by causing an increase in stomach acid.
H-2 Receptor Blockers and Proton Pump Inhibitors
H-2 receptor blockers (H-2 blockers) and Proton pump inhibitors (PPls) work by reducing the production of acid. Specifically, H-2 receptor blockers suppress the production of acid in cells lining the interior of the stomach. PPls shut down the chemical “pump” needed for stomach cells to make acid. Unfortunately, they have many known side effects.
Heart Disease
In the summer of 2007, the US Food and Drug Administration and Health Canada announced that they were looking into possible cardiac risks of popular H-2 blockers. The agencies cited two studies, which indicated a link between use of these medications and a bolstered risk of heart attack.
Pneumonia
Recent research has also suggested that using H-2 blockers and PPis up the risk of developing pneumonia and diarrhoea. The risk is increased because the function of stomach acid is not only to break down food, but also to kill pathogens. By reducing stomach acid, these drugs leave the body vulnerable to disease.[2]
Hip Fracture
Perhaps the most unusual potential side effect is hip fracture. A JAMA study proposed that PPls “may interfere with calcium absorption through induction of hypochlorhydria (low stomach acid) but they also may reduce bone resorption through inhibition of osteoclastic vacuolar proton pumps.” The study concluded that “long-term PPI therapy, particularly at high doses, is associated with an in creased risk of hip fracture.”[3]
Mental Decline
Also a real worry, some preliminary studies have found that long term use of H-2 blockers may increase the risk of mental decline in later life. The analysis, which looked at 1,558 African-Americans over age 65, found that seniors who reported “continuous use” of H-2 blockers had a 2.4-fold increased chance of some form of cognitive impairment. Researchers are unsure of the exact cause, but speculate that by blocking stomach acid, H-2 blockers interfere with the absorption of vitamin B-12, which is important for mental function[4].
Preventing heartburn naturally
Considering the possible side effects, treating heartburn with medication starts to look a lot less appealing – especially when we consider that there are numerous natural approaches which can be just as effective – here’s a few:
Lose some weight
It’s not yet clear why, but there does appear to be a relationship between heartburn and excess weight. The reason could be more complex than we yet realise, but some speculate that the extra weight of abdominal fat can simply serve to “Push” stomach acid up.
The good news is that a recent study suggested losing even just a few pounds can significantly reduce your heartburn risk.
The study concludes: “Body mass index is associated with symptoms of gastroesophageal reflux disease in both normal-weight and over weight women. Even moderate weight gain among persons of normal weight may cause or exacerbate symptoms of reflux ” [5]
Don’t stuff yourself!
Like any part of the body, the oesophageal sphincter works best when it isn’t overloaded. Its no surprise that many people experience heartburn right after a large meal, or after they’ve eaten very quickly.
As a general good point for health, you should try to eat smaller meals more often, but more slowly as much as possible, doing so will also keep pressure off the oesophageal sphincter.
Don’t hang your head!
Posture is a key element in preventing heartburn naturally. This can start with the simple act of keeping your head elevated! A study proves that head of bed elevation is a verficable, effective method for alleviating heartburn[6].
This works because it ensures that the oesophagus is higher than your stomach, as it should be. If your laying on the sofa or bed after a meal, make sure your raise your head at least 6 inches so you can sleep with head and chest elevated. A foam wedge or bricks area better choice than pillows – pillows don’t provide enough support and can put pressure on other areas of your body unnecessarily.
Ideally, don’t lie down until two to three hours after you eat.
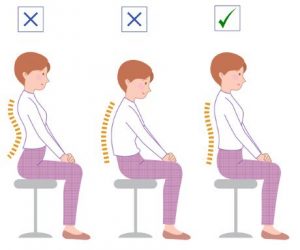
Poor posture leads to heartburn
Like any part of the body, your organs need a certain amount of space to work – your arms cant work well if you’re wrapped up in a blanket, and your digestive can’t work well if your abdomen or neck is compressed or contorted! [7]
Such as the normal flow of the digestion process from the stomach to the intestines. This reduction in normal flows or increases in back flow increases the chances for the stomach acid to enter the oesophagus causing the burning sensation.
It follows from this and the previous point that an upright and correctly seated posture during and after eating will reduce the symptoms of heartburn.
Many of us eat and sit after eating with a slouched forward posture – unfortunate this compacts the chest and stomach compartments creating the blockages previously discussed[8], so sit up straight!
Get a chiropractic check-up
A slouched forward posture might be a consequence of poor sitting habits – but it’s also frequently related to spinal misalignment, weak muscles or muscle imbalances. In these instances, you’ll probably be slouching and promoting heartburn without even realising it.
Thankfully, these misalignment and weaknesses are exactly the kinds of problems we’re ideally positioned to help resolve at complete chiropractic. An appropriate treatment plan comprised of chiropractic adjustments, postural exercises and some targeted stretches can completely eliminate heartburn if your problem is postural in nature.
[1] Lancet 2006 ;367:2086-100.
[2] JAMA 2004;292: 1955-60.
[3] JAM A 2006;296:2947-53.
[4] J Am Geriatr Soc 2007 ;55: 1248-53.
[5] N E n g l J M e d 2006 ;354:2340-8.
[6] Arch Intern Med 2006; 166:965-71.
[7] Effects of Posture on Gastro-Oesophageal Reflux. Stanciu C. Bennett J.R. Digestion 1977;15:104–109 (DOI:10.1159/000197991).
[8] Effects of posture on gastric emptying and satiety ratings after a nutritive liquid and solid meal. Theresa A. Spiegel , Harry Fried , Christine D. Hubert , Steven R. Peikin , Jeffry A. Siegel , Louis S. Zeiger. American Journal of Physiology – Regulatory, Integrative and Comparative Physiology. Published 1 August 2000. 279no. 2, R684-R694